Rheumatoid arthritis: what to know and what to do right now
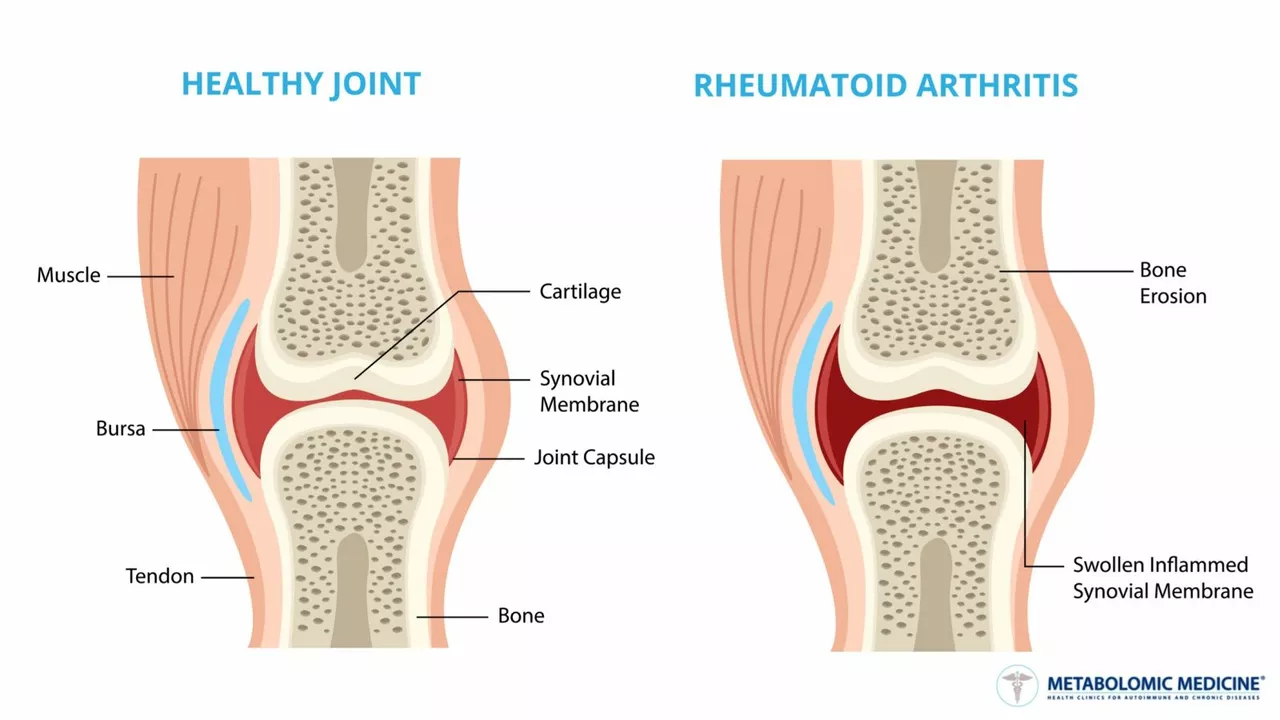
Rheumatoid arthritis (RA) is an autoimmune disease that mainly hits the joints. It often causes pain, stiffness, and swelling, usually in both hands or both knees. RA can show up at any age, and about 1% of adults have it. That makes it common enough to learn practical ways to live better with it.
Worried your joint aches are more than wear-and-tear? Look for morning stiffness that lasts over 30 minutes, swollen joints that come and go, and fatigue that doesn’t match your activity level. If these symptoms sound familiar, a blood test for rheumatoid factor or anti-CCP plus a doctor’s exam can speed up diagnosis. Early treatment matters — the sooner you start, the better your chance to stop joint damage.
How RA is treated
Treatment focuses on stopping inflammation and protecting joints. Doctors usually start with DMARDs (disease-modifying anti-rheumatic drugs) like methotrexate. Biologic drugs and newer targeted therapies help when DMARDs alone don’t control symptoms. For flare-ups, short steroid courses can calm things down fast. Over-the-counter pain relievers and topical options may ease symptoms, but they don’t stop the disease — that’s why disease-modifying meds are key.
Medication comes with trade-offs. Check for interactions, watch your bloodwork, and keep up with vaccines your doctor recommends. If medication side effects pop up, tell your clinician — small changes often fix big problems.
Simple daily tips that actually help
Move in a way that’s gentle but regular: walking, swimming, and low-impact strength work keep joints flexible and muscles strong. Joint protection matters — use larger joints for lifting, try jar openers or long-handled tools, and pace tasks to avoid flare triggers. Sleep and stress affect inflammation, so aim for consistent sleep and quick stress-breaks like a 5-minute walk or breathing exercise.
What about diet? No single “RA diet” cures the disease, but an anti-inflammatory pattern helps many people. Try more fish, vegetables, whole grains, and fewer processed foods. If smoking’s in your life, quitting is one of the best choices for slowing RA progression.
Plan for flare-ups: keep an action list (meds, icing, rest), stock easy meals, and use assistive tools when needed. Regular follow-ups with a rheumatologist keep treatment on track — don’t skip them even when you feel OK.
If joint swelling, new nodules, or sudden weakness appear, contact your doctor right away. RA can be managed well for most people when you act early, use the right meds, and adopt small daily habits that protect your joints.
Want specific tips tailored to your situation? Ask your healthcare team about medication options, physical therapy, and safe exercise plans that match your needs.
TNF Inhibitors and Cancer Risk: What You Need to Know About Biologics and Immunosuppression
TNF inhibitors help control autoimmune diseases but raise questions about cancer risk. Learn what the latest data shows about skin cancer, lymphoma, and whether etanercept is safer than adalimumab - with real-world guidance for patients.
The Relationship Between Osteoporosis and Rheumatoid Arthritis
As a blogger, I recently delved into the relationship between osteoporosis and rheumatoid arthritis. It turns out that these two conditions are closely connected, as rheumatoid arthritis can increase the risk of developing osteoporosis. This is due to the inflammation caused by rheumatoid arthritis, which can lead to bone loss and reduced bone density. Additionally, certain medications used to treat rheumatoid arthritis can also contribute to osteoporosis. It's crucial for individuals with rheumatoid arthritis to monitor their bone health and take preventive measures to protect against osteoporosis.