Bone Health: Simple Steps to Stronger Bones
Weak bones often show up as a broken wrist or hip — not a warning sign. You can protect your bones with small, daily changes: the right food, smart movement, a few checks with your doctor, and by avoiding things that speed bone loss. This guide gives clear, practical steps you can use now.
What damages and what helps
Things that speed bone loss: smoking, heavy drinking, long-term steroid use, some stomach acid drugs (PPIs), and inactivity. Age, low body weight, early menopause and a family history of fractures raise your risk. On the flip side, getting enough calcium and vitamin D, doing weight-bearing and resistance exercise, and keeping active protect bone strength.
Calcium targets: most adults need 1,000 mg a day; women over 50 and everyone over 70 should aim for 1,200 mg. Try to get calcium from food first — milk, yogurt, sardines, tofu, and leafy greens. If you use supplements, don’t exceed recommended doses and split them through the day if needed.
Vitamin D helps your body use calcium. A common starting point is 800–1,000 IU daily, but a blood test is the best way to know your level. If you’re deficient, your doctor may suggest a higher short-term dose.
Quick daily habits for stronger bones
Move with purpose: do 30 minutes of weight-bearing activity most days — brisk walking, jogging, dancing, hiking, or stair climbing. Add two sessions a week of strength work: bodyweight moves, dumbbells, or resistance bands. Balance and flexibility exercises — tai chi or single-leg stands — cut fall risk.
Food and supplements: prioritize calcium-rich meals first. If you take a calcium supplement, separate it from thyroid medicine by 4 hours. Keep antibiotic timing in mind: calcium can block absorption of tetracyclines and fluoroquinolones — leave 2–4 hours between them.
Cut toxic habits: quit smoking, limit alcohol to one drink a day for women and two for men, and avoid very low-calorie diets that strip nutrients.
Home safety: remove loose rugs, add non-slip mats in bathrooms, keep stairs well lit, and wear supportive shoes indoors. Have your vision checked and review medicines with your pharmacist for ones that cause dizziness.
When to see your doctor
If you’re a woman 65 or older, a man 70 or older, or anyone with a fracture after a minor fall, ask about a bone density (DXA) scan. If the scan shows low bone density, treatments range from oral bisphosphonates (like alendronate) to injections (denosumab) or newer options for severe cases. Each drug has pros and cons — for example, bisphosphonates should be taken on an empty stomach with a full glass of water and you must stay upright for 30–60 minutes to avoid irritation.
If you use long-term steroids or have other risk factors, don’t wait. Talk with your doctor about testing, vitamin D checks, and a plan that matches your risk and lifestyle. Small changes now prevent big problems later.
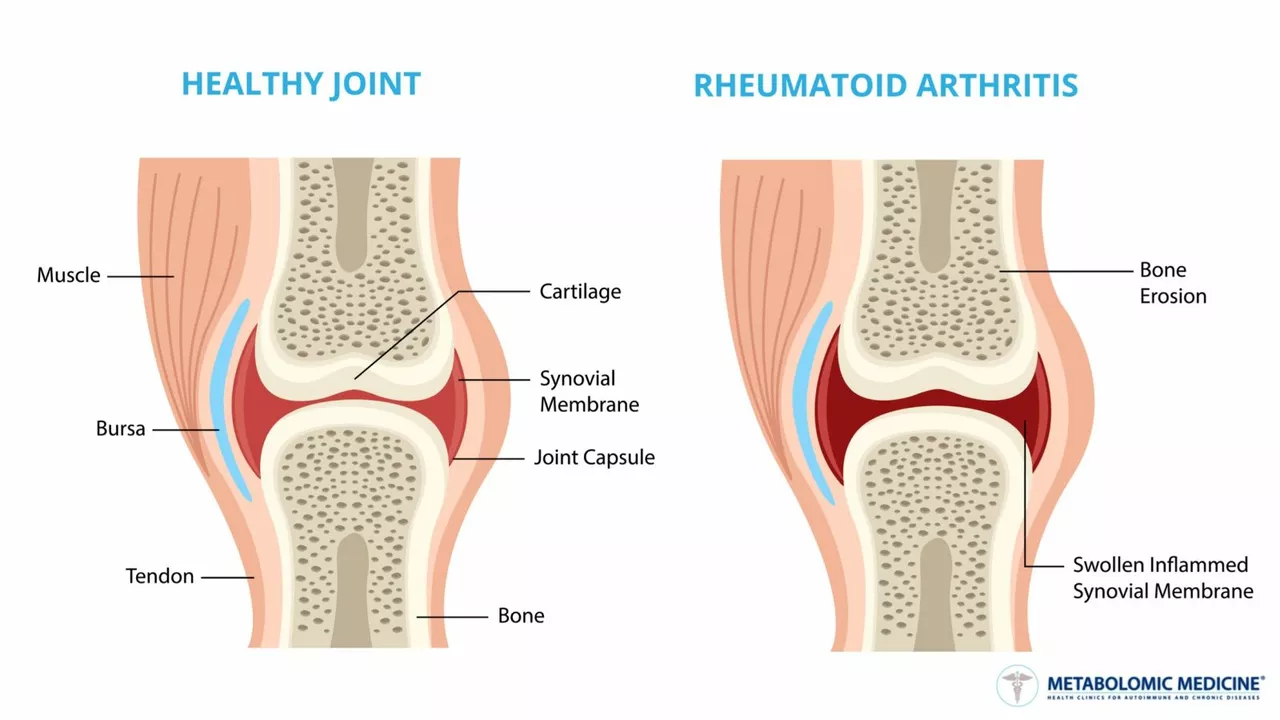
The Relationship Between Osteoporosis and Rheumatoid Arthritis
As a blogger, I recently delved into the relationship between osteoporosis and rheumatoid arthritis. It turns out that these two conditions are closely connected, as rheumatoid arthritis can increase the risk of developing osteoporosis. This is due to the inflammation caused by rheumatoid arthritis, which can lead to bone loss and reduced bone density. Additionally, certain medications used to treat rheumatoid arthritis can also contribute to osteoporosis. It's crucial for individuals with rheumatoid arthritis to monitor their bone health and take preventive measures to protect against osteoporosis.