Osteoporosis: Practical Guide to Prevention, Diagnosis, and Treatment
Breaking bones from a simple fall isn't inevitable—osteoporosis makes bones fragile, but you can do a lot to prevent and treat it. This page collects clear, useful advice so you know what to check, what to change, and when to get help.
Osteoporosis means bone density is low and the bone structure weak. Men and women both get it, but women after menopause have higher risk. Age, long-term steroid use, smoking, heavy drinking, low body weight, and certain illnesses or meds raise the chance. Family history also matters.
How doctors diagnose it
The most common test is a DEXA scan, which measures bone mineral density. Results come as T-scores: -1.0 or above is normal, -1.0 to -2.5 is osteopenia, and -2.5 or lower is osteoporosis. Blood tests may follow to check calcium, vitamin D, thyroid, and kidney function. If you’ve had a low-trauma fracture—say a break from a minor fall—tell your doctor right away.
Everyday steps that help
Nutrition matters. Aim for about 1,000–1,200 mg of calcium a day from food or supplements if your diet falls short. Get vitamin D tested; many adults need 800–2,000 IU daily or more if levels are low. Focus on dairy or fortified plant milks, leafy greens, canned salmon with bones, and small dairy-free sources like almonds. Supplements are fine when food isn’t enough.
Move your body. Weight-bearing exercise—walking, stair climbing, light jogging, dancing—and muscle-strengthening exercises build bone and cut fall risk. Try balance work like tai chi or heel-to-toe walking. Aim for two strength sessions weekly and daily short walks.
Quit smoking and limit alcohol. Smoking speeds bone loss. Keep alcohol to no more than one drink a day for women and two for men; excess drinking weakens bone and coordination.
Medications can be game-changers. Bisphosphonates (alendronate, risedronate) lower fracture risk and are often first-line. Denosumab is an injection given every six months. Bone-building drugs like teriparatide or romosozumab are options for severe cases. Each drug has pros, cons, and safety checks—discuss risks and monitoring with your clinician.
Make your home safer. Remove loose rugs, add grab bars in the bathroom, improve lighting, and wear shoes with grip. Small changes cut the chance of a fall and a bad break.
When to see a doctor: after any low-impact fracture, if you have major risk factors, or if you’re age 65+ (women) or 70+ (men), ask about a DEXA scan. If you’re on long-term steroids or have conditions like rheumatoid arthritis, schedule an earlier check.
Finally, keep a simple record: medication list, bone density results, vitamin D level, and any fractures. That makes follow-up easier and helps you and your doctor make the right choices fast.
Ask about side effects and duration. Some treatments need drug holidays or monitoring of kidney and jaw health. If you have dental work planned, tell your dentist before starting certain injections or IV drugs. Also check with your doctor about supplements and other meds to avoid interactions. Keep asking questions.
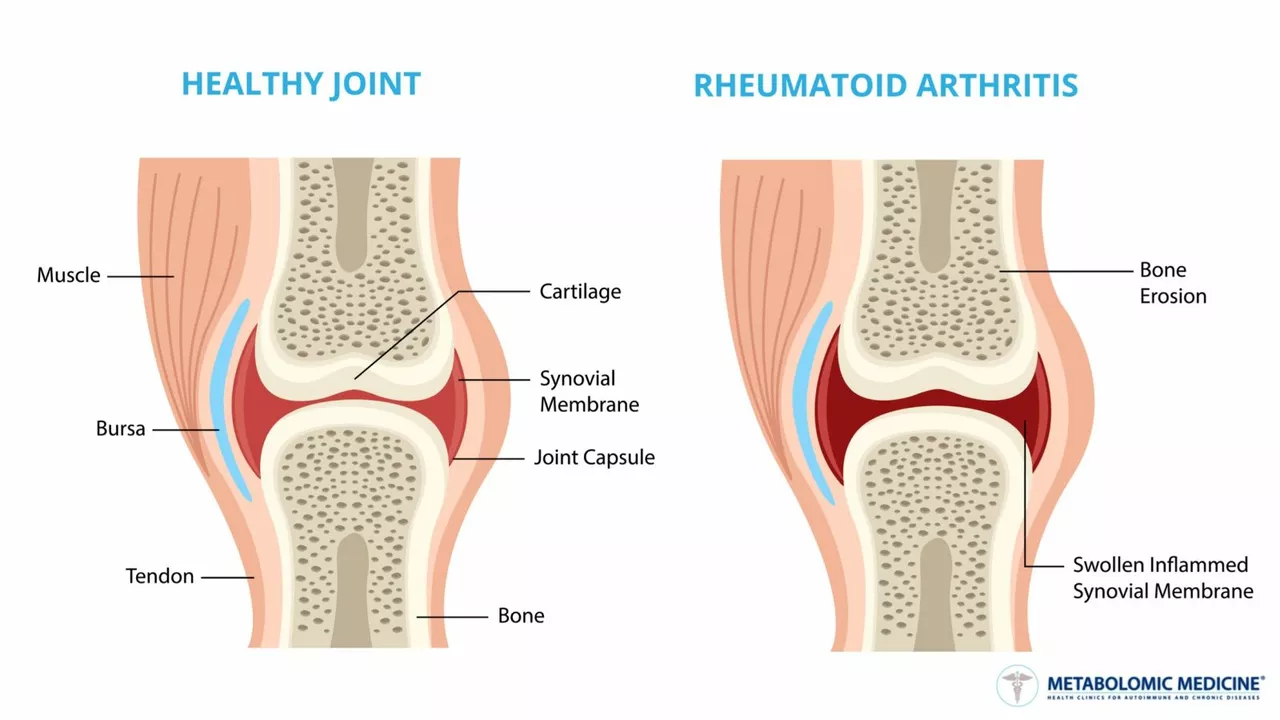
The Relationship Between Osteoporosis and Rheumatoid Arthritis
As a blogger, I recently delved into the relationship between osteoporosis and rheumatoid arthritis. It turns out that these two conditions are closely connected, as rheumatoid arthritis can increase the risk of developing osteoporosis. This is due to the inflammation caused by rheumatoid arthritis, which can lead to bone loss and reduced bone density. Additionally, certain medications used to treat rheumatoid arthritis can also contribute to osteoporosis. It's crucial for individuals with rheumatoid arthritis to monitor their bone health and take preventive measures to protect against osteoporosis.