Meniere's disease: simple guide to symptoms and management
Meniere's disease causes sudden spinning attacks (vertigo), a feeling of fullness in one ear, ringing (tinnitus), and changes in hearing. Attacks can last from 20 minutes to several hours and leave you exhausted. You don't have to guess what to do next—read down for clear signs, testing, treatment options, and everyday tips that can help.
What you might notice first: sudden intense vertigo, nausea, sweating, and difficulty standing up. Hearing may go up and down in the affected ear. Tinnitus often comes with a blocked or full feeling. Between attacks some people feel fine, while others have mild imbalance or a steady low-level ringing.
What causes it and how it's diagnosed
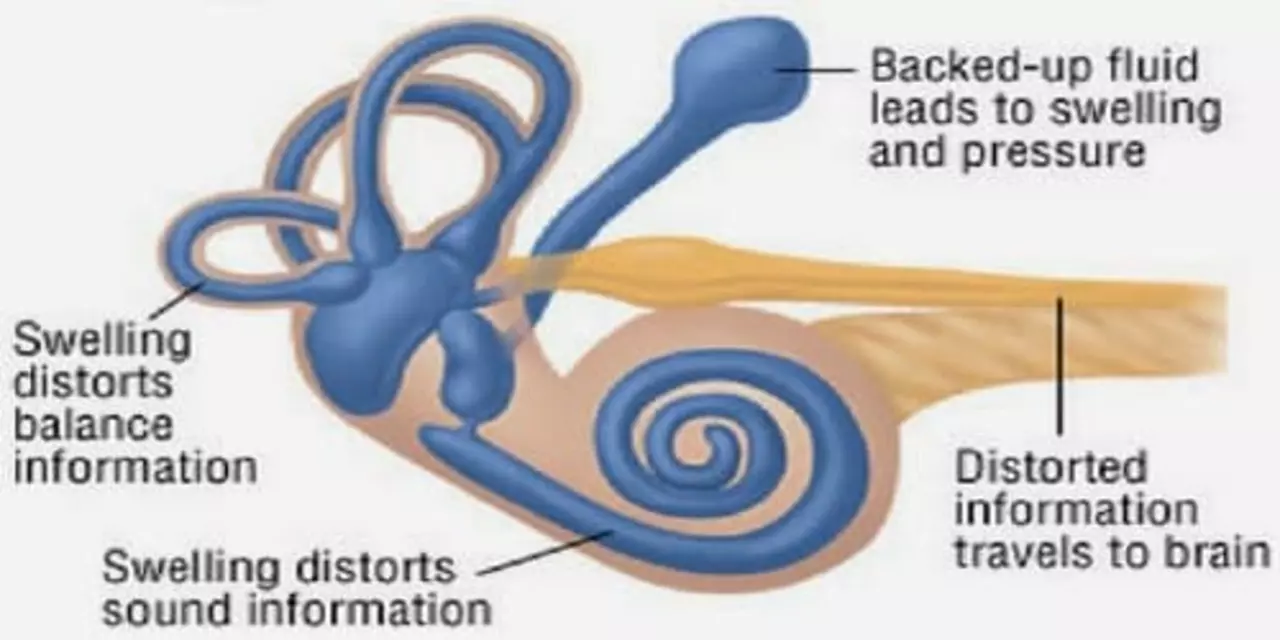
Doctors think Meniere's results from extra fluid (endolymph) in the inner ear, but the exact reason varies—salt balance, poor fluid drainage, viral triggers, or genetics can play a role. Your doctor will ask about attack patterns and do a hearing test (audiogram). They may use balance tests (VNG or ENG) and sometimes an MRI to rule out other problems like a vestibular schwannoma. Diagnosis is based on your symptoms and test results, so keep a simple diary of episodes—duration, symptoms, and possible triggers.
Practical treatment and self-care
There is no one-size-fits-all cure, but many people get better control. Start with lifestyle steps: cut salt (aim for modest reduction, not extreme restriction), limit caffeine and alcohol, and stay hydrated. Stress and poor sleep can make attacks worse, so prioritize regular sleep and simple stress relief like short walks or breathing exercises.
Medications can help during attacks and to reduce their frequency. For sudden vertigo your doctor may prescribe vestibular suppressants (meclizine or a short course of diazepam) and anti-nausea drugs. Long-term options include low-dose diuretics, betahistine where available, or steroid injections into the middle ear to calm inflammation. If symptoms keep getting worse, stronger options like intratympanic gentamicin or surgery to decompress or shunt the inner ear are considered, but those are for severe cases only.
Hearing loss can become permanent. Use hearing aids or assistive devices early if hearing is affecting daily life. Balance physical therapy (vestibular rehab) helps many people recover stability between attacks. Simple home safety steps—non-slip mats, good lighting, and sitting down at the first sign of spinning—reduce fall risk.
When to see a doctor: if you have your first major vertigo attack, sudden hearing loss, frequent or longer attacks, or trouble walking. Keep good notes on spells and share them with your clinician. With the right plan many people reduce how often attacks happen and keep a normal life.
During an attack sit or lie down, close eyes, and focus on a fixed spot to help the spinning pass. Avoid driving until symptoms stop. Keep anti-nausea or vestibular meds handy if prescribed. Ask your doctor how often to get hearing tests—usually yearly or more if hearing changes. Finding a local support group or online community helps with practical tips and reduces the stress of dealing with attacks.
The Impact of Meniere's Disease on Daily Life and Activities
Meniere's Disease has greatly impacted my daily life and activities in several ways. Firstly, the unpredictable episodes of vertigo often leave me feeling disoriented and unable to perform simple tasks. Secondly, the constant ringing in my ears (tinnitus) can be quite distracting, making it difficult for me to focus on conversations or work. Additionally, the fluctuating hearing loss has affected my ability to communicate effectively with others, causing frustration and isolation. Overall, Meniere's Disease has significantly disrupted my daily routine and interactions, leaving me constantly searching for ways to manage and cope with its symptoms.